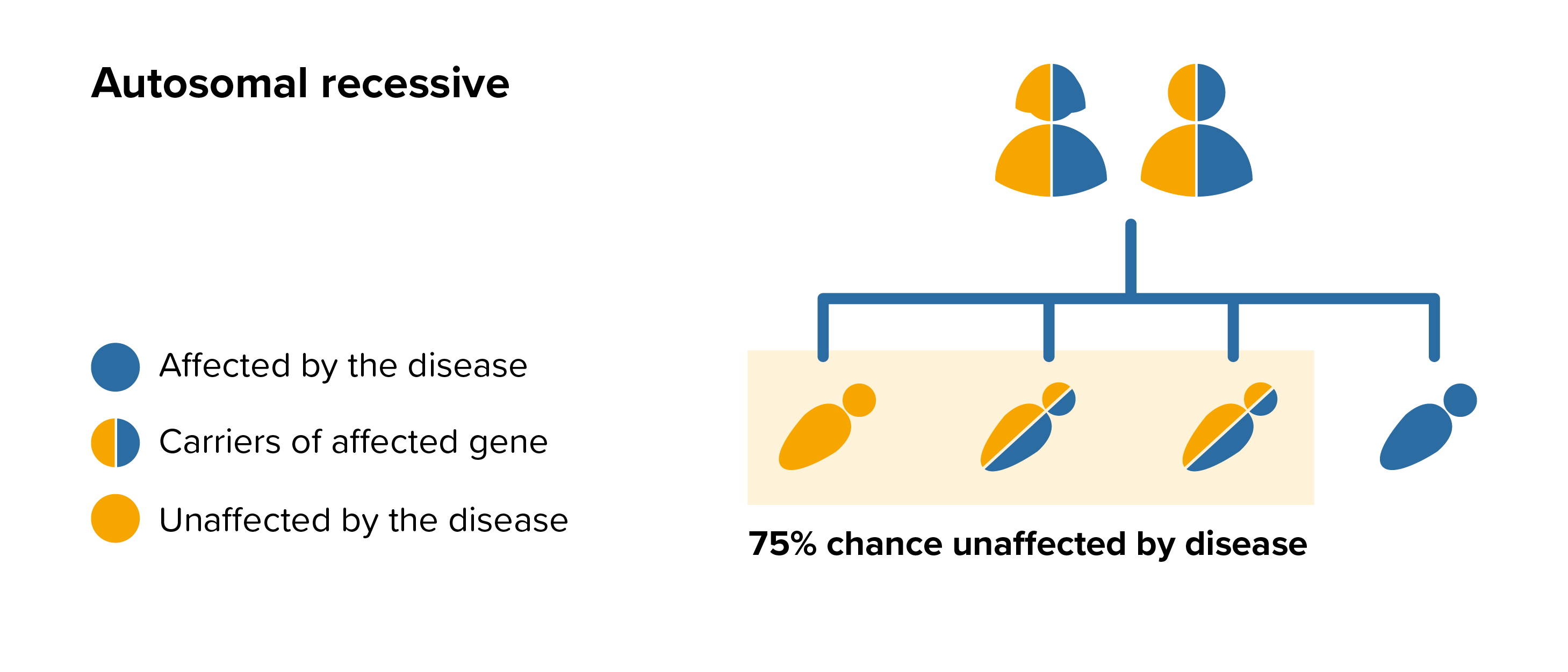
The speed of progression of AGU varies between people, development is typically normal throughout childhood with signs and symptoms beginning around the age of 2 or 3 usually with delayed speech.
Appearance
Children with AGU may be tall for their age but lack of a growth spurt in puberty typically causes adults to be short. Although the body is in proportion, stature becomes restricted and the abdomen tends to protrude. Other changes in appearance develop gradually as oligosaccharides accumulate.
People with AGU tend to have similar facial features that include widely spaced eyes, small ears, full lips and the nose is short and broad with a flattened bridge. The face is usually square shaped with an asymmetric skull and the neck is often short.
The skin is generally thicker than normal which is the reason for wrinkles being a physical characteristic of the disease. Folds of skin over the inner corner of the eyes are common in babies and may remain, over time the cheeks tend to sag. A rash of small red spots which is known as angiokeratoma has been observed on the legs and feet of some patients.
Brain
People with AGU will experience deteriorating brain related symptoms because of the effect of accumulation of oligosaccharides in the brain. Learning difficulties have been consistently observed, these are usually mild in the early years but can become severe by the time the child is 5 to 7 years old. Intellectual disability progressively worsens in adolescence. Speech development becomes progressively delayed and most people lose much of the speech they have learned resulting in a few words by adulthood. Movements and actions of the muscles usually deteriorate by adulthood and many will experience reduced muscle tension.
Some people with AGU may experience hydrocephalus, which is water on the brain. This can happen because the fluid that protects and circulates around the brain and spinal cord may become blocked over time. The blockage causes increased pressure in the head which can press on the brain causing headaches and delayed development. Tests to confirm hydrocephalus can be done using a CT or MRI scan, or a lumbar puncture. If hydrocephalus is confirmed it can be treated by an insertion of a small tube in the spinal cord which drains fluid from the brain.
Heart
The size of the heart in people with AGU can be abnormally large and storage of oligosaccharides in the heart will cause some damage to the heart valves. Heart murmurs can happen when heart valves become damaged by stored oligosaccharides. The heart valves are designed to keep blood flowing in the right direction. If a valve is weakened or changed in shape it may not work properly and a small amount of blood may leak in the wrong direction. Some people may develop problems with one of the heart valves but they may have valvular heart disease for years without any ill effects.
An electrocardiogram (ECG) test is used to identify problems with heart muscle, function and valves, it is a painless procedure and is often carried out annually (or as often as the doctor thinks necessary) to show whether any problems are starting.
Lungs
Normally the ribs are curved and between the ribcage and breastbone there is flexibility for the chest to move freely. In AGU the chest cannot move freely to allow the lungs to take in a large volume of air because the ribs are straight and there is limited flexibility between the ribcage and breastbone. The muscles at the base of the chest may be pushed upwards by an enlarged liver and spleen, further reducing the space for the lungs. Additionally, the tissue of the lungs becomes thickened by stored oligosaccharides and stiffer than usual. This leads to an increase in secretions which are harder to clear as the restricted lungs make it difficult to take a deep enough breath to cough properly. When the lungs are not fully cleared there is an increased risk of infection which can lead to scarring causing further obstruction.
Medication for controlling cough and cold symptoms and mucus production is available but it is essential to consult the doctor rather than using ‘over the counter’ medication which may not help. Medications such as antihistamines may dry out the mucus making it thicker and harder to dislodge. Decongestants usually contain stimulants that can raise blood pressure and narrow blood vessels, both are undesirable effects for people with AGU. Cough medicines that have a sedating effect may cause more problems with sleep apnoea by depressing muscle tone and respiration. It is common for people with AGU to develop secondary bacterial infections which should be treated with antibiotics.
Liver, Spleen and Abdomen
The liver and spleen become enlarged because they are storing oligosaccharides. The enlarged liver does not cause problems or lead to liver failure however the size can interfere with eating and breathing. The enlarged liver and spleen coupled with weakness of the tummy (abdominal) muscles can lead to a hernia. A hernia is when an organ, such as the intestine, pushes through a weak spot in the muscle that holds it in place. Treatment options differ depending on the type of hernia, in some cases surgery is needed.
Bones and joints
The spine bones (vertebrae) of people with AGU are poorly shaped resulting in the spine twisting called scoliosis. The top bone of the spine holding the skull in place is often underdeveloped, the neck can therefore be fragile and shorter than usual. The skeleton may also become deformed and bone and cartilage can form in abnormal places. These changes are normally identified through X-rays to diagnose problems. People with AGU have bones that become progressively weak and prone to fracture and often an unusually large range of joint movement in. Sometimes children have ‘knock knees’ resulting in their feet being forced progressively further apart. Bones in the feet become malformed and this can make the leg bones predisposed to breaking.
People with AGU often experience pain, weakness or loss of feeling in the fingertips, this is caused by thickening of the ligaments which causes pressure on the nerves. It is called carpal tunnel syndrome and can be relieved by an operation. An electrical test called a nerve conduction study can show whether carpal tunnel syndrome is the cause
Ears
Some degree of deafness is common in people with AGU. It may be conductive deafness, nerve deafness or both (called mixed deafness) and can be made worse by frequent ear infections.
Conductive deafness is when sound waves that travel through the ear canal, drum and the middle ear are impaired. Correct functioning of the middle ear depends on the pressure behind the ear drum being the same as that in the outer ear canal and the atmosphere. This pressure is kept equal by the eustachian tube which runs from the middle ear to the back of the nose. If the eustachian tube is blocked the pressure behind the eardrum will drop and the transmission of sound waves will be impaired. If this persists, fluid from the lining of the middle ear will build up and in time will become thick like glue, hence the condition being known as glue ear. Glue ear can be treated through surgery by inserting a small ventilation tube called a grommet, however these can fall out quickly and T-tubes, a type of grommet which stays in place longer, are an alternative option.
Nerve deafness is damage to the tiny hair cells in the inner ear. It may happen at the same time as conductive deafness, in which case it is referred to as mixed deafness. Mixed deafness can be managed by grommets or hearing aids. Nerve deafness is managed by fitting hearing aids in most people. More severely affected children may keep pulling out their hearing aids at first, but it is important to persevere at wearing them so that communication can be maintained. Alternatives include radio aids and the loop system which can be helpful at school and at home.
Eyes
People with AGU experience clouding of the cornea which is caused by stored mucopolysaccharides and can lead to significant visual disability. Some people cannot tolerate bright lights as the clouding causes bending of the light which affects the vision, tinted glasses may be helpful in such circumstances. Severe corneal clouding may reduce sight, especially in dim light, a loss of night vision is common, cornea transplants can be a treatment option.
Dental
Good dental hygiene is very important for children with AGU, teeth should be well cared for to avoid tooth decay, pain and extractions. Usually teeth are widely spaced and poorly formed with fragile enamel. Cleaning around the mouth with a small sponge or a stick soaked in mouthwash will help keep the mouth fresh and avoid bad breath.